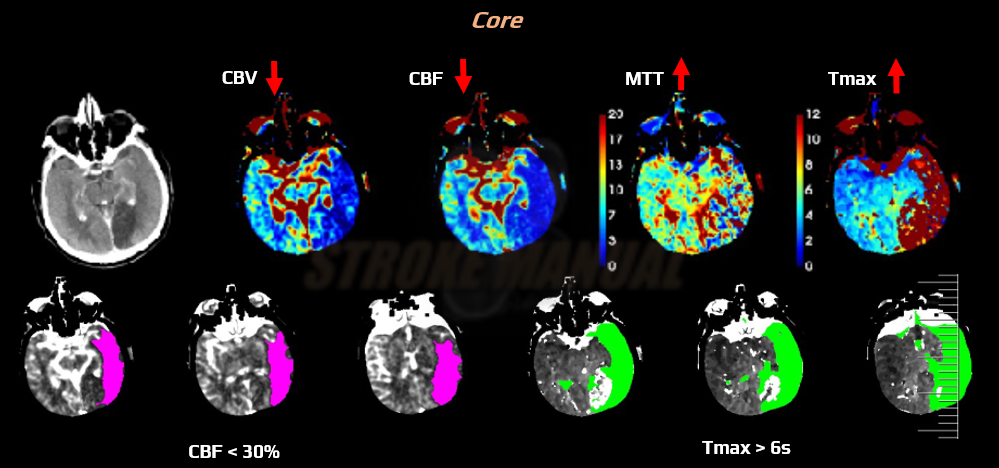
Assuming a normal distribution of differences between umbilical venous and arterial pH, the upper limit of the 95 th percentile range is 0.10 (see Case 5).(3,4) Finding a pH difference greater than 0.10 suggests either cord occlusion with terminal bradycardia or chronic fetal heart failure with terminal bradycardia. Using the data published by Yeomans, Hauth, Gilstrap, and Strickland (2), the average pH difference is 0.07 (7.35 minus 7.28 = 0.07). However, it seems safe to assume that a difference of 4 mmol/L or more is significant.īecause pH is the most reproducible of the three measured blood gas parameters, looking at the difference between pHs to alert to an abnormally large difference is most helpful. There is no general agreement on the definition of a widened base deficit difference. However, because lactic acid crosses the placenta poorly (1), a greater base deficit in the arterial cord blood sample indicates the presence of umbilical vein occlusion with at least some interval of partially restored umbilical arterial blood flow. With intact umbilical-placental circulation, any metabolic acidosis appearing in the umbilical artery will almost instantaneously appear in the umbilical vein. Widened differences also may be associated with fetal heart failure. The hallmark of cord occlusion with terminal bradycardia is widened venoarterial pH, PCO 2, and sometimes base deficit differences, usually associated with normal or near-normal umbilical venous cord gases. However, the differences between venous and arterial pH, PCO 2, and base deficit are greater than usual. 
The usual relationship between venous and arterial values is intact the venous pH and PO 2 are higher, and the venous PCO 2 is lower. The respiratory acidosis in the arterial sample is also mild, but there is also a mild metabolic acidosis. The respiratory acidosis in the venous sample is mild the base deficit is within normal limits. Apgar scores were 6 and 9 at one and five minutes, respectively. The umbilical cord was tight around the shoulder and body. 
The infant was then delivered by outlet forceps. The patient was taken fully dilated to the delivery room, where the FHR monitor revealed a variable deceleration to 60 bpm for 90 seconds. During labor, the FHR monitor revealed recurrent variable decelerations that were deeper and longer-lasting, and then a deceleration to 60 bpm for three minutes. Membranes ruptured spontaneously two hours prior to admission. Because of decreased fetal movement complaint three days before admission, a non-stress test was performed and was reactive, but had several mild, variable decelerations. The mother was a 26-year-old, gravida 4, para 3, aborta 0, with an intrauterine pregnancy at 40 0/7 weeks' gestation by good dates. Case 10: Umbilical Cord Occlusion with Terminal Fetal Bradycardia, Mild
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
